Introduction
Overhead athletes, particularly baseball players, subject their shoulders to extreme biomechanical demands that often result in adaptive changes over time. Following a SLAP (Superior Labrum Anterior to Posterior) repair, one of the most common impairments encountered during rehabilitation is decreased shoulder internal rotation (IR). While some loss of IR is considered a normal adaptation in throwers, excessive deficits following surgery can become pathological, delaying return to play, altering throwing mechanics, and increasing the risk of further injury.
Baseball is a highly specialized sport, with clinicians who specialize in overhead athletes. This specialization requires understanding the underlying causes and implementing a structured, evidence-based rehabilitation approach to achieve optimal recovery.
Background
In the throwing athlete, the dominant shoulder typically demonstrates increased external rotation and decreased internal rotation compared to the non-dominant side, while maintaining a relatively symmetrical total arc of motion. However, after a SLAP repair, this balance is often disrupted. Postoperative immobilization, soft tissue healing constraints, and neuromuscular guarding can all contribute to excessive stiffness, particularly in the posterior shoulder.
Posterior capsule tightness is widely recognized as a primary contributor to glenohumeral internal rotation deficit (GIRD), a condition associated with altered humeral head translation and increased stress on surrounding structures. Wilk et al. (2011) emphasized that GIRD exceeding 20 degrees, especially when accompanied by a loss of the total arc of motion, is associated with a higher incidence of shoulder pathology in overhead athletes.
In the post-SLAP repair population, trigger points commonly develop in the posterior rotator cuff (infraspinatus and teres minor), as well as in the subscapularis and posterior deltoid. Trigger points can directly contribute to decreased internal rotation by increasing passive muscle stiffness and inducing pain-mediated inhibition.
Fernández-de-las-Peñas et al. (2006) demonstrated that active trigger points in the infraspinatus are associated with reduced shoulder range of motion and altered muscle activation patterns. Similarly, Lucas et al. (2004) reported that trigger points can significantly impair muscle length and joint mobility, further compounding motion deficits already present from surgical recovery.
Athletes may present with localized tenderness, referred pain patterns into the anterior shoulder or arm, and a firm end-feel during internal rotation. These findings can complicate both assessment and treatment, as traditional stretching alone may not adequately address the neuromuscular component of the restriction. As such, a comprehensive evaluation should include not only joint range of motion and capsular mobility but also palpation for trigger points, assessment of muscle tone, and identification of pain referral patterns. Myers et al. (2006) highlighted the importance of addressing posterior shoulder soft-tissue restrictions broadly, including both capsular and muscular contributors.
Case Report
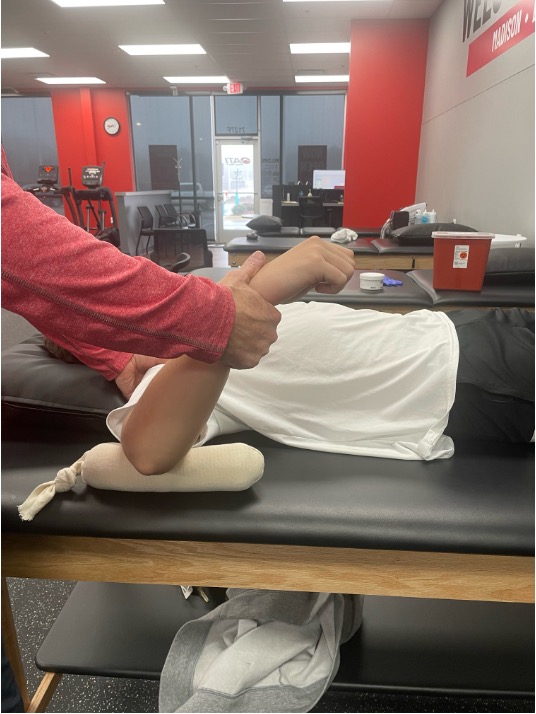
A practical illustration of this can be seen in a case involving a high school baseball pitcher presenting with posterior shoulder pain and decreased internal rotation during the late cocking and follow-through phases of throwing. The athlete demonstrated a significant loss in internal rotation compared to the non-throwing arm. The athlete was 6 months post-op and had been attending physical therapy with another provider, receiving manual joint mobilizations, soft-tissue mobilization, and posterior shoulder stretching to address the athlete’s GIRD. Following a follow-up with his physician, the patient was referred for evaluation of his loss of internal rotation. Assessment of the athlete revealed active trigger points in his infraspinatus and teres minor.
The athlete received TrP DN to both the infraspinatus and teres minor, followed by soft-tissue mobilization, horizontal adduction, and manual internal-rotation stretching during his first treatment. Immediately following treatment, the athlete had full restoration of internal rotation.
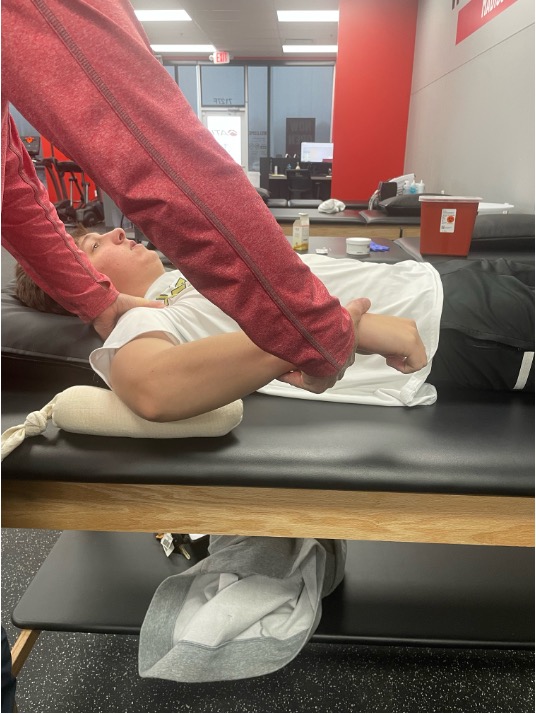
The athlete followed up with PT the following week, maintaining full shoulder internal rotation motion from the previous treatment. The athlete was again seen for repeated treatment to restore full soft-tissue mobility and flexibility of his posterior rotator cuff, with the previous treatment repeated for a total of 4 visits. The athlete was able to return to his throwing program without pain, while maintaining shoulder internal rotation range of motion.
Summary
This case study outlines the importance of addressing all possible causes of range-of-motion loss and conducting a mobility assessment. Following a single session of dry needling targeting these muscles, the athlete demonstrated an immediate improvement in internal rotation range of motion and a reduction in pain during simulated throwing movements. This rapid change highlights the significant contribution of myofascial restrictions to loss of motion and reinforces the value of incorporating trigger point interventions into the plan of care.
Treatment targeting trigger points has resulted in significant improvements in pain and function among patients with shoulder disorders, as reported by Bron et al. (2011). Dry needling has also gained support as an effective intervention, with Cummings and White (2001) demonstrating its ability to reduce trigger point sensitivity and improve range of motion, likely through both mechanical and neurophysiological mechanisms. In addition, techniques such as the cross-body adduction stretch and modified sleeper stretch remain foundational for reinforcing the newly gained range of motion through stretching and neuromuscular re-education, but they are often more effective once trigger point-related resistance has been reduced. McClure et al. (2007) demonstrated that the cross-body stretch is particularly effective in improving posterior shoulder mobility, especially when soft-tissue restrictions are addressed concurrently.
This case study outlines the importance of considering all potential causes of range-of-motion restrictions following surgical intervention, including trigger points. Decreased shoulder internal rotation following SLAP repair is a multifactorial impairment, with myofascial trigger points potentially playing a significant role alongside capsular tightness and neuromuscular dysfunction. Incorporating targeted trigger point assessment and treatment—particularly dry needling—can lead to meaningful, sometimes immediate, improvements in range of motion and symptoms. By addressing both the mechanical and neuromuscular contributors to loss of motion, clinicians can better support baseball athletes in achieving a safe, high-level return to performance.
Todd Hooks, PT, ATC, OCS, SCS, MOMT, MTC, CSCS, CMTPT, NREMT-1, FAAOMPT – Instructor
References
Bron, C., de Gast, A., Dommerholt, J., Stegenga, B., Wensing, M., & Oostendorp, R. A. (2011). Treatment of myofascial trigger points in patients with chronic shoulder pain: a randomized controlled trial. BMC Medicine, 9(8).
Cummings, T. M., & White, A. R. (2001). Needling therapies in the management of myofascial trigger point pain: a systematic review. Archives of Physical Medicine and Rehabilitation, 82(7), 986–992.
Fernández-de-las-Peñas, C., Alonso-Blanco, C., & Miangolarra, J. C. (2006). Myofascial trigger points in subjects presenting with mechanical neck pain: a blinded, controlled study. Manual Therapy, 11(3), 256–263.
Lucas, K. R., Polus, B. I., & Rich, P. A. (2004). Latent myofascial trigger points: their effects on muscle activation and movement efficiency. Journal of Bodywork and Movement Therapies, 8(3), 160–166.
McClure, P., Balaicuis, J., Heiland, D., Broersma, M. E., Thorndike, C. K., & Wood, A. (2007). A randomized controlled comparison of stretching procedures for posterior shoulder tightness. Journal of Orthopaedic & Sports Physical Therapy, 37(3), 108–114.
Myers, J. B., Laudner, K. G., Pasquale, M. R., Bradley, J. P., & Lephart, S. M. (2006). Glenohumeral range of motion deficits and posterior shoulder tightness in throwers. The American Journal of Sports Medicine, 34(3), 385–391.
Wilk, K. E., Macrina, L. C., Fleisig, G. S., Porterfield, R., Simpson, C. D., Harker, P., Paparesta, N., & Andrews, J. R. (2011). Correlation of glenohumeral internal rotation deficit and total rotational motion to shoulder injuries in professional baseball pitchers. The American Journal of Sports Medicine, 39(2), 329–335.

